Major depressive disorder (MDD) stands as a pervasive and debilitating global health crisis, recognized as a primary driver of disability worldwide. Despite advancements in psychiatric care, a significant subset of individuals, approximately 30% of those diagnosed, grapple with treatment-resistant depression (TRD). This condition is characterized by a persistent lack of adequate symptom improvement with conventional antidepressant medications, leaving many in a state of ongoing suffering. In recent years, ketamine has emerged as a beacon of hope, demonstrating remarkable rapid antidepressant effects for patients with TRD. However, the precise molecular mechanisms by which ketamine exerts its influence within the complex landscape of the human brain have remained largely elusive, hindering efforts to refine and personalize this promising therapeutic approach.
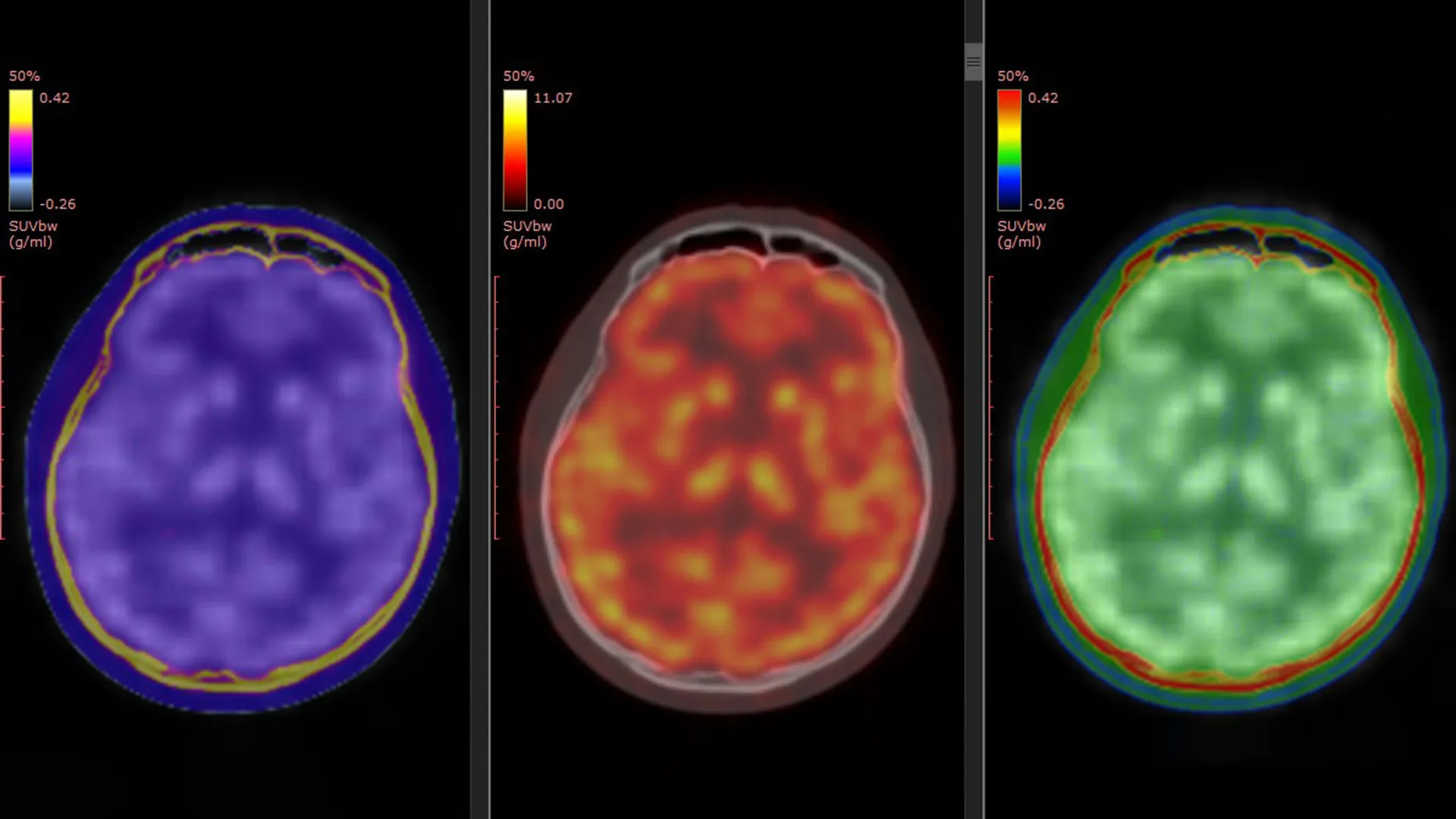
A groundbreaking study, published on March 5, 2026, in the esteemed journal Molecular Psychiatry, has significantly advanced our understanding of ketamine’s neurobiological underpinnings. Spearheaded by Professor Takuya Takahashi of the Department of Physiology at Yokohama City University Graduate School of Medicine in Japan, the research team employed a sophisticated positron emission tomography (PET) imaging technique. This cutting-edge methodology allowed for the direct observation of changes in glutamate $alpha$-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid receptors (AMPARs) in living human brains. AMPARs are critical proteins that govern synaptic plasticity and glutamatergic signaling, processes intrinsically linked to neuronal communication and the modulation of mood in individuals undergoing ketamine treatment.
Professor Takahashi articulated the significance of their findings, stating, "Although ketamine has shown rapid antidepressant effects in patients with treatment-resistant depression, its molecular mechanism in the human brain has remained unclear. Our research provides the first direct visual evidence of how ketamine influences these crucial brain receptors in humans, bridging a critical gap in our knowledge."
Illuminating Brain Receptors: The Power of a Novel PET Tracer
The success of this pivotal research hinges on a specialized PET tracer, designated as [$^11$C]K-2, previously developed by Professor Takahashi’s team. This innovative tracer possesses the unique capability to visualize cell-surface AMPARs directly within the active human brain. Prior investigations, conducted in both laboratory settings and animal models, had strongly suggested a role for AMPAR activity in mediating ketamine’s antidepressant effects. The current study, however, represents the first empirical demonstration of this phenomenon occurring in human subjects, providing compelling evidence to corroborate earlier hypotheses.
To execute this ambitious research, the investigators meticulously collated data from three registered clinical trials conducted in Japan. The comprehensive study cohort comprised 34 patients formally diagnosed with treatment-resistant depression and 49 healthy individuals who served as a control group, establishing a baseline for comparison. Over a two-week treatment period, the participating patients were administered either intravenous ketamine or a placebo. PET brain imaging was conducted at two key junctures: immediately preceding the commencement of treatment and again following the final infusion. This meticulous temporal design enabled researchers to precisely track and compare alterations in AMPAR levels and their distribution within the brain throughout the course of the intervention.
Region-Specific Brain Changes Correlate with Symptom Relief
The analytical findings revealed a striking pattern of widespread abnormalities in AMPAR density among individuals with TRD when compared to their healthy counterparts. Crucially, these discrepancies were not uniformly distributed across the entire brain but were instead concentrated in specific neuroanatomical regions.
Further analysis demonstrated that ketamine did not induce uniform modifications in AMPAR density throughout the brain. Instead, the observed improvements in depressive symptoms were intrinsically linked to dynamic, region-specific adjustments in AMPAR levels. In certain cortical areas, a notable increase in AMPAR density was observed, suggesting enhanced neuronal signaling in these regions. Conversely, reductions in AMPAR density were detected in brain areas associated with reward processing, most notably the habenula. These finely tuned, region-specific shifts in AMPAR distribution exhibited a strong correlation with the amelioration of patients’ depressive symptoms, underscoring their pivotal role in ketamine’s therapeutic efficacy.
Professor Takahashi elaborated on these critical observations: "Ketamine’s antidepressant effect in patients with TRD is mediated by dynamic changes in AMPAR in the living human brain. Using a novel PET tracer, [$^11$C]K-2, we were able to visualize how ketamine alters AMPAR distribution across specific brain regions and how these changes correlate with improvements in depressive symptoms." These findings offer direct human evidence that substantiates previously proposed mechanisms derived from animal studies and concretely links them to tangible clinical antidepressant outcomes.
A Potential Biomarker for Predicting Treatment Response
Beyond elucidating the intricate mechanisms of ketamine’s action, these findings hold significant promise for practical clinical applications. The ability to visualize AMPAR density via PET imaging could potentially evolve into a valuable biomarker. Such a biomarker would empower clinicians to more accurately assess and predict individual patient responses to ketamine treatment for TRD.
The imperative to identify reliable biological markers that predict treatment response is paramount in mental health care, particularly given the substantial proportion of patients who do not achieve remission with standard antidepressant therapies. The current study represents a significant stride towards achieving this critical objective, offering a tangible tool for precision medicine in psychiatry.
Paving the Way for More Personalized Depression Treatments
By enabling scientists to directly observe AMPAR activity within the living human brain, this research effectively bridges a persistent chasm between foundational laboratory discoveries and their translation into clinical practice. The results unequivocally identify AMPAR modulation as a central mechanism underpinning ketamine’s rapid antidepressant effects. Furthermore, they strongly suggest that AMPAR PET imaging could serve as a cornerstone for developing more individualized and effective treatment strategies for individuals grappling with TRD in the future.
This pioneering work has the potential to accelerate the development of more precise and targeted therapies, offering renewed hope and improved outcomes for countless individuals living with the profound challenges of treatment-resistant depression. The implications extend beyond ketamine, potentially informing the development of new therapeutic agents that target AMPARs or related glutamatergic pathways.
Broader Context and Future Directions
The global burden of depression is staggering. The World Health Organization (WHO) estimates that depression affects over 280 million people worldwide. In 2019, depression was the leading cause of disability globally, contributing significantly to the overall burden of disease. The economic costs are also immense, with studies estimating annual costs of depression in the hundreds of billions of dollars due to lost productivity and healthcare expenditures. Treatment-resistant depression, in particular, poses a significant challenge, often leading to prolonged suffering, increased risk of suicide, and a substantial drain on healthcare resources.
The advent of ketamine as a rapid-acting antidepressant has been a significant development in addressing this unmet need. First synthesized in the 1960s, ketamine was initially used as an anesthetic. Its antidepressant properties were serendipitously discovered in the late 1990s and have since been the subject of intense research. Unlike traditional antidepressants that often take weeks to show effects and primarily target monoamine systems (serotonin, norepinephrine, dopamine), ketamine’s rapid action is thought to be mediated by the glutamatergic system, particularly through its effects on NMDA receptors and downstream AMPAR activation.
The timeline of research leading to this pivotal study is a testament to scientific perseverance. Early preclinical studies in the early 2000s began to explore ketamine’s antidepressant potential. By the late 2000s and early 2010s, clinical trials started to confirm its efficacy in TRD. However, the precise neural mechanisms remained a subject of debate and investigation. The development of the [$^11$C]K-2 PET tracer by Professor Takahashi’s group represented a critical technological advancement, enabling the direct visualization of AMPARs in humans, a feat not previously possible with such specificity. The integration of data from multiple clinical trials, as performed in this study, adds robustness and generalizability to the findings.
The implications of this research are far-reaching. The identification of AMPAR density as a potential biomarker could revolutionize how TRD is diagnosed and treated. Currently, treatment decisions for TRD are largely empirical, involving sequential trials of different medications and therapies. A biomarker that predicts response to ketamine could allow clinicians to more rapidly identify suitable candidates, potentially reducing the time to effective treatment and minimizing exposure to ineffective therapies. This could lead to improved patient outcomes, reduced healthcare costs, and a more efficient allocation of resources.
Moreover, the findings provide a deeper understanding of the neurobiological underpinnings of depression itself. The observation of region-specific AMPAR abnormalities in TRD suggests that the disorder is not a monolithic entity but rather involves distinct neurobiological profiles. This nuanced understanding could pave the way for the development of novel therapeutic targets beyond AMPARs, potentially leading to entirely new classes of antidepressants.
While the study offers immense promise, it is important to acknowledge that further research is needed to fully validate the use of AMPAR PET imaging as a clinical biomarker. Larger, more diverse patient populations will need to be studied to confirm the reliability and generalizability of these findings. Additionally, research into the long-term effects of ketamine and the sustainability of AMPAR changes in response to treatment will be crucial.
The collaborative nature of this research, supported by substantial funding from various Japanese governmental and scientific bodies including the Ministry of Education, Culture, Sports, Science and Technology, the Japan Agency for Medical Research and Development (AMED), and the Japan Society for the Promotion of Science (JSPS), highlights the national commitment to advancing mental health research. Foundations such as the Takeda Science Foundation and the Keio Next-Generation Research Project Program also underscore the broad support for innovative scientific endeavors.
In conclusion, the work by Professor Takahashi and his team represents a significant leap forward in our understanding of treatment-resistant depression and the therapeutic potential of ketamine. By providing direct visual evidence of ketamine’s action on AMPARs in the human brain, this study not only demystifies a complex biological process but also offers tangible pathways toward more personalized and effective treatments for millions affected by this debilitating condition. The future of depression treatment may well be illuminated by the insights gained from visualizing these critical brain receptors.